Case Report | DOI: https://doi.org/10.31579/2835-8465/037
Autologous Platelet-Rich Plasma (APRP) as an Adjunct for Enhanced Electric Burn Wound Healing: A Case Report
1 Junior Resident, Department of Surgery, JIPMER, Puducherry, India – 605006.
2 Department of Plastic Surgery & Telemedicine, JIPMER, Pondicherry, India – 605006.
3 Senior Resident, Department of Plastic Surgery, JIPMER, Puducherry, India – 605006.
4 Senior Resident, Department of Orthopaedics, Karpaga Vinayaga Institute of Medical Sciences and Research Center, Tamil Nadu, India – 603308.
*Corresponding Author: Ravi Kumar Chittoria, MCh, DNB, MNAMS, FRCS (Edin), FRCS(Glasgow), FAMS, FTSI, FRSM, FACS, DSc, PhD, MBA; Senior Professor and Associate Dean (Academic); Head of IT Wing and Telemedicine; Department of Plastic Surgery and Telemedicine, JIPMER, Puducherry,
Citation: Siddhartha Raj, Ravi Kumar Chittoria, Kanav Gupta, and Nagarjun S Ghatti, (2025), Autologous Platelet-Rich Plasma (APRP) as an Adjunct for Enhanced Electric Burn Wound Healing: A Case Report, Orthopaedics Case Reports. 4(6); DOI: 10.31579/2835-8465/037
Copyright: © 2025, Dr. Ravi Kumar Chittoria. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: 31 October 2025 | Accepted: 03 November 2025 | Published: 17 November 2025
Keywords: Autologous Platelet Rich Plasma (APRP); wound healing; burns; electric burns
Abstract
This article explores the utilization of Autologous Platelet-Rich Plasma (APRP) as a supplementary treatment for electrical burns. Given its abundance in diverse growth factors, APRP holds significant promise as an adjunctive therapy to enhance outcomes across various plastic surgery procedures. This case report highlights the beneficial effects of APRP in expediting the wound healing process in a patient with electric burns.
Introduction
Wound healing is a complex and highly coordinated biological process involving multiple overlapping stages. Optimal healing necessitates the intricate interplay of various cellular components and growth factors, among which platelets play a crucial role. Extensive research has firmly established the significance of platelets in promoting wound healing by releasing essential growth factors. Beyond growth factor release, platelets also facilitate the secretion of bioactive proteins that attract key cells such as macrophages, mesenchymal stem cells, and osteoblasts, thereby aiding in the removal of necrotic tissue and fostering robust tissue regeneration [1].
Autologous Platelet-Rich Plasma (APRP) has emerged as a valuable therapeutic tool for expediting wound healing. Platelet-Rich Plasma (PRP) is characterized by its significantly elevated platelet concentration, alongside a rich assortment of clotting factors and growth factors [3]. APRP, specifically, boasts remarkably higher levels of vital growth factors like Platelet-Derived Growth Factor (PDGF), Transforming Growth Factor-beta (TGF-β), Vascular Endothelial Growth Factor (VEGF), Epidermal Growth Factor (EGF), and Fibroblast Growth Factor (FGF) compared to normal plasma. This heightened concentration of growth factors in APRP directly enhances tissue regeneration and accelerates healing processes.
Given its remarkable properties in tissue repair and regeneration, APRP is increasingly recognized as an adjunct therapy for various conditions in plastic surgery. This discussion underscores the significance of APRP as a supplemental treatment modality, particularly in the context of electrical burn wound management.
Materials and Methods
This research was conducted at a Tertiary Care Centre within the Department of Plastic Surgery, following approval from the department's ethical committee. Informed consent was duly obtained from the patient.
The subject of this study was a 14-year-old male with a history of accidental electrical burns (5% TBSA) with B/L rib fractures and spine fracture. The patient initially presented to a nearby hospital where preliminary resuscitation was performed, and he was subsequently referred to our centre. He arrived with a delay of approximately 10 hours’ post-injury. APRP was employed as an adjuvant therapy for wound healing in this patient.
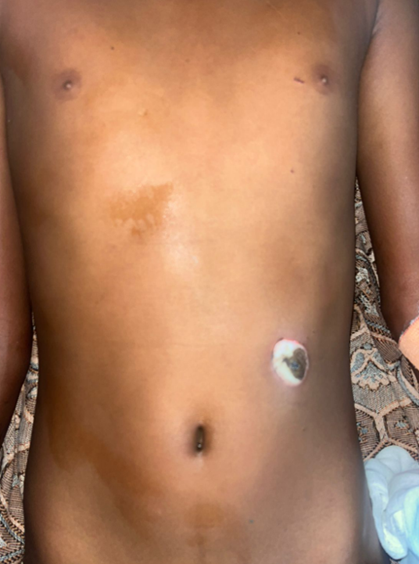
Figure 1 showing condition of electrical burns on the abdomen.
APRP was prepared using a standard and validated technique as described by Li, Weivei et al. With sterile precautions and after obtaining informed consent, 45 ml of whole blood was drawn from a peripheral vein. To this, 5 ml of 3.2% Sodium Citrate was added, bringing the total volume to 50 ml (maintaining a blood to anticoagulant ratio of 9:1).
The blood mixture was then transferred to a centrifugation tube and placed into a centrifuge. The solution underwent a first centrifugation step at 3000 rpm for 10 minutes. Following this, three distinct layers were observed: an upper portion containing plasma and platelets, a middle portion (buffy coat) containing white blood cells (WBCs) with platelets, and a lower portion containing red blood cells (RBCs). The middle (buffy coat) and lower (RBCs) portions were carefully discarded.
The upper portion (plasma and platelets) was then transferred to a new sterile tube for a second centrifugation step at 4000 rpm for 10 minutes. This yielded two distinct portions: the upper two-thirds containing platelet-poor plasma (PPP), and the lower one-third containing platelet-rich plasma (PRP), which included erythrocyte with platelet clumps. The lower one-third portion, representing the APRP, was then harvested for therapeutic use.
For this patient, subcutaneous injection of APRP was administered circumferentially around the wound margin using a 23G needle (Figure 2). The application process is depicted in (Figure 3)

Figure 2 shows APRP injection.
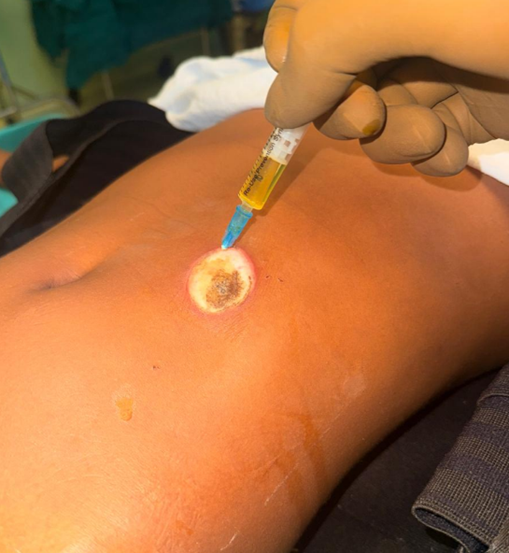
Figure 3 showing application of APRP.
Results
Wound healing was found to be hastened by application of APRP, proving the efficacy of using APRP in treatment for wound healing (Figure 4).
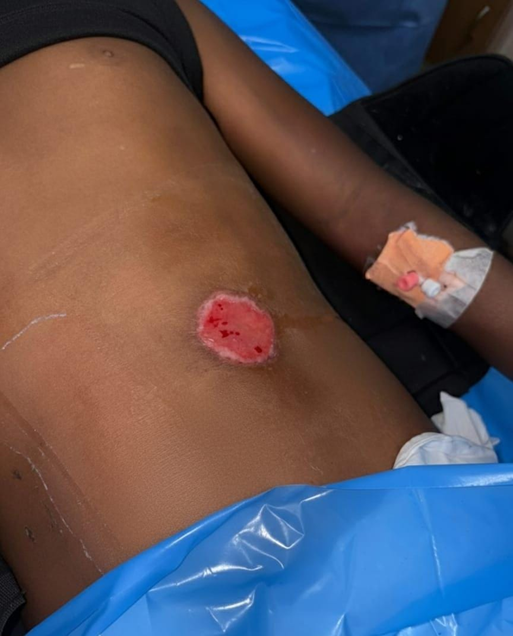
Figure 4: Post APRP.
Discussion
Autologous platelet-rich plasma (APRP) is derived from the patient's own blood and contains a higher platelet count compared to the peripheral blood [1]. Initially utilized for treating thrombocytopenia, its applications expanded to various medical fields, notably sports medicine for musculoskeletal injuries. In wound management, APRP addresses the impediment to healing caused by low platelet count and high protease activity. By supplying growth factors, APRP promotes mitogenic, angiogenic, and chemotactic actions [2], aiding chronic wound healing. Furthermore, APRP fosters the deposition of TYPE I collagen, potentially beneficial for scar management3. Activation of APRP, typically achieved with calcium salts [4,5,6], yields heightened concentrations of growth factors like PDGF and VEGF. However, the volume of APRP obtained from a patient's blood poses a limitation, especially for treating large wounds, necessitating careful consideration. Additionally, administering APRP may pose challenges on uneven surfaces, affecting its uptake efficiency [7,8].
Conclusion
APRP proves beneficial in promoting wound healing across a spectrum of cases, regardless of whether they are acute or chronic and irrespective of their underlying causes. Its utility extends to burn injuries as well as within the realm of cosmetic surgery. Our case report findings affirm that APRP contributes to enhanced wound healing across diverse wound types.
References
- 1. Rubina Alves, Ramon Grimalt. A review of plateletrich plasma: History, biology, mechanism of action, 4:18-24.
View at Publisher | View at Google Scholar - 2. Padmalakshmi Bharathi Mohan, Saurabh Gupta, Ravi Kumar Chittoria, Abhinav Aggarwal, Chirra Likhitha Reddy, Imran Pathan, Shijina Koliyath. (2020), Autologous Platelet-rich Plasma Enriched Pixel Grafting. Journal of Cutaneous and Aesthetic Surgery, Volume 13, Issue 4, October-December 2020.
View at Publisher | View at Google Scholar - 3. Barbara Hersant, Mounia Sid Ahmed-Mezi, Romain Bosc, Jean-Paul Meningaud. (2017), Autologous Platelet Rich Plasma/Thrombin Gel Combined with Split Thickness Skin Graft to Manage Postinfectious Skin Defects: A Randomized Controlled Study. Adv Skin Wound Care. 2017 Nov; 30(11):502-508.
View at Publisher | View at Google Scholar - 4. Claudia S Cohn, Evelyn Lockhart. (2015), Autologous platelet-rich plasma: evidence for clinical use. Curr. Opin. Hematol. 2015 Nov; 22(6):527-532.
View at Publisher | View at Google Scholar - 5. Sudhanva H.K., Panday S, Chittoria RK, Mohapatra DP, Friji MT, Dinesh KS. (2016). Role of APRP in the successful uptake of Split Skin Graft. Dermatology international Volume 1 number 2 July to December 2016.
View at Publisher | View at Google Scholar - 6. Elankumar S, Sudhanva H.K., Abhinav A, Chittoria R.K. (2017), APRP spray devices: a novel technique of applying APRP. Dermatology international Volume 2 number 2, July to December 2017.
View at Publisher | View at Google Scholar - 7. Weibrich G, Kleis WK, Hafner G, Hitzler WE, (2002), Growth factor levels in platelet- rich plasma and correlation with donor age, sex and platelet count. Journal of cranio-maxillofacial surgery. 2002; 30(2):97-102.
View at Publisher | View at Google Scholar - 8. Yuan T, zhang CQ, Tang MJ, Guo SC, Zeng BF. (2009), Autologous platelet- rich plasma enhances healing of chronic wounds. Wounds. 2009; 21(10):280-285.
View at Publisher | View at Google Scholar

 Clinic
Clinic
